Remote Medical Scribe Services
Electronic Medical Records (EMR) adoption demands the need to have the medical assistant all the time during the examination of the patient by the physician so that each and every detail is entered into EMR real time. Also, the absenteeism of the medical assistants makes the ‘physicians’ day tough. On top of these, many patients object to an assistant being present while they are being examined. Seyyone can offer practices with quality virtual/remote scribe solutions who can create charts real time and avoid the awkwardness of having an assistant present during examination.
Workflow for Seyyone’s medical scribe services
Plan A
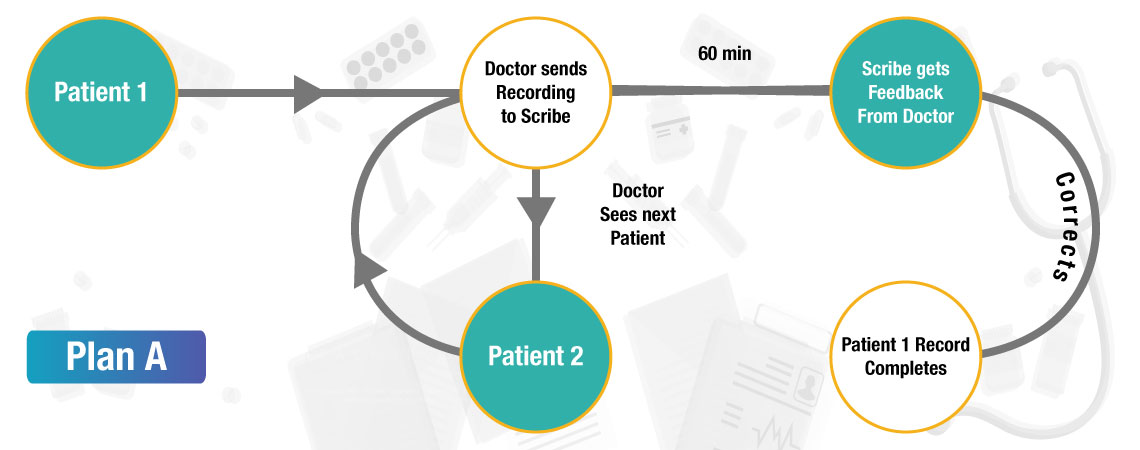
Requirements
- A digital voice recorder for the physician to record the dictation at the end of each consultation or the doctor may choose to use a toll-free line to record the dictation.
- A mic connected to the computer/laptop installed with Skype app or a smartphone installed with Skype app (the scribe will use Skype app for conversation with the physician).
Plan B
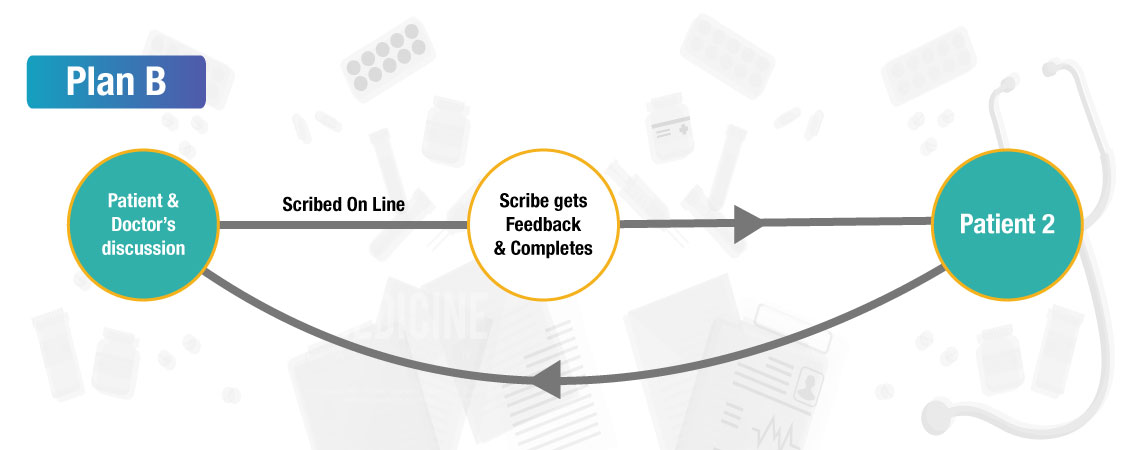
Requirements
- A smartphone installed with Skype app for communication between Scribe and physician.
- A mic connected to the computer/laptop installed with Skype app, the scribe will be listening to the conversation between physician and patient via this mic.